The gastric bypass is a surgical procedure in obese patients that is used to bypass and thus exclude large parts of the stomach and the small intestine from the digestive process. With a small remaining stomach the patients feel satiety even after a very limited amount of food. The result is a fast and pronounced weight loss.
Gastric bypass (more precisely: Roux-en-Y gastric bypass) is a very common obesity surgery used to reduce weight. It is named after the Swiss surgeon César Roux, who developed the basic technique for the intervention. The "Y" represents the Y-shaped diagram of the way the intestinal sections are joined together.
Gastric bypass has been performed on 17,215 patients since 2005. There was a clear preference for laparoscopic access, over which 98.6% of the procedures were performed. Patients with RYGB (47.92 kg / m2) had a significantly lower BMI than patients with other procedures (50.27 kg / m2).
The success of a gastric bypass surgery is based on two principles:
- The stomach reduction decreases the food intake (restriction)
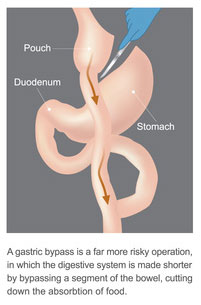
- Due to the elimination of the important upper part of the small intestine (duodenum), the digestive juices that break down food are mixed later with the food pulp (lower nutrient absorption = malabsorption)
The weight loss after a gastric bypass surgery is dramatic and reliable, but it is accompanied with some lifelong restrictions: Patients with a Reoux-en-Y-bypass may eat only very small portions, because after the operation the remaining stomach ("stomach pouch") has a very small volume. The poor nutrient utilization means that patients have to take life-long dietary supplements and vitamins (especially vitamin B12, trace elements and protein preparations) to avoid deficiency symptoms. Some of the nutrients remain undigested causing fermentation processes in the colon. However, the operation cannot be reversed after a successful weight reduction.
Gastric bypass is one of the most widely used and established methods of achieving significant weight reduction through surgery. Here, similar to the tubular stomach, the stomach is significantly reduced, so that much less food can be absorbed (restrictive component). Unlike the sleeve or stomach, however, the residual stomach is not completely removed, but remains in the body and produces digestive juices. In addition, the small intestine is redirected (bypass) so that food and digestive juices can mix later in the small intestine. Therefore, a part of the calories (fats and sugars) can not be digested, but leaves the body again with the stool. The reduced intake of calories, fats and nutrients is called malabsorption. Due to this mode of action, experts also refer to this procedure as a malabsorptive procedure or as a restrictive malabsorptive procedure.
The reduced absorption of the body for sugar, fats and other nutritional components promotes weight loss. At the same time, however, many nutrients, vitamins and trace elements can be ingested by the organism due to this surgical measure. This may require an additional intake of dietary supplements or mineral and vitamin supplements. For this purpose, every six months, check-ups should take place at the family doctor or in our center. The method known by many as 'gold standard' has been used by us since 2007. Again, similar to the other methods, a decision for or against this is very individual and can only take place in personal consultation.
There are also different methods of this procedure, which usually differ in the length of the different small intestine areas (loops). But also the size of the smaller stomach (pouches) can vary. In our center we inform you in great detail about the advantages and disadvantages of the different variants.
Omega loop bypass (also called "Mini" Bypass)
It is a variant of the gastric bypass and also a combined restrictive malabsorptive procedure.
The advantage of this method is a shorter operating time and risk reduction because of the saving of a suture connection in contrast to the Roux-Y-bypass and a possibly greater weight loss. Critics point out that there is an increased risk of ulcer formation and possibly also in the long-term course of carcinoma formation at the suture connection between stomach and small intestine, caused by the contact between bile juice and gastric mucosa. However, this presumption, based on decades of experience in gastric surgery, has not yet been proven in the medium-term follow-up periods.
The Omega Loop Bypass differs from the standard bypass in that it creates a slightly larger gastric pouch, which is then connected to the jejunum (ulcer) 200 to 250 cm after it starts. For this, the small intestine does not have to be severed. The dining passage thus bypasses parts of the stomach, the duodenum and the first 200-250 cm small intestine.
Because of the described problem we practice in our obesity center a modified method that prevents the contact between bile and gastric mucosa.
Preparation to gastric bypass surgery
Any pathological changes in the stomach need to be ruled out before the operation. This makes necessary a stomach examination for diseases such as gastric mucosal inflammation or gastric ulcers and for possible bacterial colonization with "Helicobacter pylori", which can cause gastric ulcers. In addition to a gastroscopy and the examination of the gastric juices, an ultrasound of the upper abdomen is also used to detect gallstones. These are removed in the course of gastric bypass surgery as they can lead to inflammation of the gallbladder and bile duct.
Gastric bypass surgery procedure
The gastric bypass surgery lasts about 90 to 150 minutes depending on the patient and is performed under general anesthesia. The surgery usually requires a hospital stay of about one day before the operation (surgical and anesthesia preparation) plus five to seven days after it. After the gastric bypass surgery, you will not be able to work for three weeks.
Gastric bypass is now performed almost exclusively using the so-called minimally invasive surgery. This technique, also known as the keyhole method, does not require a large abdominal incision. Instead, the instruments and a small camera are introduced into the abdominal cavity through several two centimeters long skin cuts. Minimally invasive operations generally have lower surgical risk compared to open operations and are therefore particularly suitable for obese patients who are already more vulnerable to complications during and after surgery.
Gastric bypass surgery consists of several stages:
- After the induction of general anesthesia, the surgeon makes several skin incisions to insert the instruments and the camera with a light source into the abdominal cavity. After that, gas (usually CO₂) is introduced into the abdominal cavity to lift the abdominal wall from the organs giving the surgeon more space in the abdomen and a better view of the organs.
- Then the stomach is cut off just below the esophagus using a special surgical stapler. The stapler cuts and clamps simultaneously so that the cut edges are closed immediately. Thus, only a small remaining stomach (the so-called gastric pouch or stomach pouch) is left at the end of the esophagus. It has a volume of less than 50 milliliters. The remaining stomach is left in the body but it is closed at the upper end and thus quasi "shut down".
- The next step is to cut the small intestine in the area of the so-called jejunum. The lower end of the cut is now pulled up and sewn to the stomach pouch. This connection is sometimes called gastrojejunal anastomosis.
- Then further below the remaining cut end of the jejunum is sewn with the third small intestine section ("ileum"), so that the Y-shape is formed (y-anastomosis). Only here the digestive juices from the duodenum (bile and pancreatic secretion) are mixed with the food pulp.
Who is gastric bypass suitable for?
The gastric bypass is suitable for people with a body mass index (BMI) of more than 40 kg/m² (Obesity Grade III or morbid obesity). In any case, the condition for a gastric bypass surgery is that all non-operative measures were not sufficiently successful even after six to twelve months. These measures include, for example, professional nutritional advice, exercises and behavioral therapy (multimodal concept for obesity, MMC).
To have a gastric bypass performed you should be at least 18 and not more than 65 years old. However the intervention is possible in younger or older people in individual cases. Gastric bypass surgery is particularly recommended for people whose excess weight is caused by consumption of rich in calories food (sweets, fats) and drinks. This type of food is broken down badly, and the body can utilize it only to a small extent storing it as body fat.
If metabolic diseases, such as diabetes mellitus, hypertension or a sleep apnea syndrome, are already caused by obesity, a gastric bypass surgery can already be performed in patients with a BMI of 35 kg/m².
Various physical and mental illnesses prohibit an obesity operation such as gastric bypass. A gastric bypass surgery cannot be performed after previous surgeries or in case of stomach malformations, gastric ulcers and addictions, as well as untreated eating disorders such as binge eating or bulimia. Pregnant women also have to forgo gastric bypass surgery.
Effectiveness of gastric bypass surgery
Gastric bypass is a very effective procedure, even though only few patients achieve normal weight (BMI ≤ 25 kg/m²). Studies have shown that in the long term a weight loss of about 60 to 70 percent of the excess weight is possible with a gastric bypass, i.e. the amount of weight that separates obese patients from the people with normal weight.
The weight loss after a gastric bypass operation has not only purely cosmetic effect, it also favorably impacts the metabolism. For example, in many cases, an existing diabetes mellitus is greatly improved and sometimes even cured. In many cases, blood glucose levels fall short after the operation, although the patient has not yet lost much weight. The reasons for this are yet unclear. It is suspected that various hormonal changes are set in motion by the operation (for example, such hormones as ghrelin, glucagon, GIP, etc.), which favorably affects the metabolism.
Advantages of gastric bypass surgery
Since the gastric bypass surgery combines two principles (restriction and malabsorption, see above), the procedure is extremely effective even if the patient's obesity is caused by excessive intake of liquid or soft high calorie food. For these so-called "sweet-eaters" the sole reduction of the stomach volume achieved through a gastric banding, gastric balloon or sleeve gastrectomy, would not be sufficient.
Side effects
Some side effects are associated with gastric bypass. Their strength differs in each individual case and therefore cannot be predicted. The most important side effects:
- Digestive disorders caused by malabsorption: flatulence, abdominal pain, nausea, bloating
- Iron deficiency and anemia: Most of the dietary iron is usually ingested in the duodenum. The gastric bypass diverts the food from the duodenum making the iron intake more difficult. The iron deficiency is prevented by additional iron intake.
- Vitamin B12 deficiency (special form of anemia): Vitamin B12 is absorbed in the last section of the small intestine (terminal Ileum). However, this process requires an auxiliary, the so-called intrinsic factor, which is produced by the stomach. The gastric bypass, however, diverts the food from the stomach and thus less intrinsic factor is formed. Vitamin B12 must therefore be regularly injected intramuscularly or into the vein. Vitamin B-12 supplements are also available, which can be absorbed directly by the oral mucosa (sublingual application). However, their effectiveness is still discussed.
- Vitamin D deficiency: why is gastric bypass causing a vitamin D deficiency is yet unclear. Vitamin D can be easily taken in with food (orally).
- Dumping syndrome: A number of symptoms (dizziness, nausea, diaphoresis or palpitation), which are caused by an instantaneous (sudden) dumping of food from the esophagus directly into the small intestine, are referred to as dumping syndrome. It happens because the stomach pouch lacks the lower stomach sphincter (porter). In the small intestine, the osmotic forces make the food pulp absorb water from the surrounding tissues and blood vessels. This reduces the amount of fluid in the circulatory system, which can result in a blood pressure drop. A dumping syndrome occurs mainly after drinking very sugary beverages or eating fatty food.
- Gastric ulcer in the stomach pouch: After gastric bypass surgery, the risk of a stomach pouch ulcer is increased. To cope with it the patient must take acid-reducing drugs, the so-called proton pump inhibitors (PPI), permanently, if a gastric ulcer occurred after a gastric bypass operation.
- Loss of muscle mass: a fast weight loss is often associated with a loss of muscle mass because the organism tries to compensate for the relative deficiency of carbohydrates by degrading body proteins (mainly from less important muscle cells). Regular physical training can halt this side effect. Easy on the joints sports such as light weight training, cycling, swimming or aqua-jogging are especially advisable for obese people.
Gastric bypass: Risks and complications
Gastric bypass is a large abdominal surgery that greatly alters the normal anatomy of the gastrointestinal system. In principle, surgical risks are low, but complications cannot be ruled out as with any surgical procedure. Non-specific surgical risks include:
- Anesthetic complications
- Organ and vascular injuries with bleeding
- Infections of internal and external wounds
- Leaks of artificial organ connections (anastomoses) with risk of inflammation of the peritoneum (peritonitis)
- Wound healing disorders
- Disturbances of normal gastrointestinal movements (intestinal atonia)
Gastric bypass: Nutrition after surgery
Nutritional recommendations after gastric bypass surgery
Persons after gastric bypass surgery require regular follow - up care in the obesity surgery therapy experienced doctor and a nutritionist. In the first year after the operation four follow-up appointments should take place, then once a year. By checking the intake level and nutrient composition using nutritional protocols, nutrient deficiencies can be prevented by timely intervention. Laboratory controls with determination of the blood count and selected parameters of vitamins, minerals and
Trace elements are used to diagnose deficiency states. If the values are below the norm, nutrient supplements must be prescribed (according to the European Recommended Daily Allowance, EU-RDA). A nutrient deficiency is more likely the more invasive a procedure is. Gastric banding or gastric tube scarcity often causes deficiencies in care, but gastric bypass and biliopancreatic diversion (BPD) are almost always absent. The supplements must then be taken a lifetime!
Gastric bypass: Costs
The cost of a gastric bypass differs considerably depending on the clinic. It ranges approximately between 6,500 and 15,000 euros.
























 Loading ...
Loading ...


