Nowadays in Germany as well as in other countries bypass surgery is one of the most efficient ways of treating ischemic heart disease caused by coronary vessel constriction and reduction of heart oxygen supply. Ischemic heart disease in a neglected condition can result not only in stenocardia, but also in lethal cardiac infarction. Therefore, well-timed and correct treatment sustains patient’s life and improves its quality.
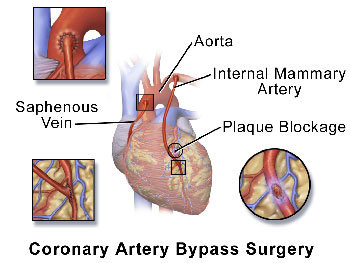
Ischemic heart disease treatment in Germany depends on how neglected the disease is. Medicinal treatment is usually assigned at the initial stages of the disease; it is aimed at vasodilatation of damaged vessels which improves heart oxygen and blood supply. At later stages it is possible to use angioplasty treatment (vasodilatation of constricted vessels with the help of a cylinder and possible stent installation. In case it is not possible to use such sparing techniques, German experts suggest a bypass surgery. Heart catheterization conducted with the use of advanced medical technologies (bypass) allows preliminary estimation of the disease scale. Bypass surgery is suggested in case it is expected to give better results than medicinal treatment or angioplasty.
Coronary 3-vessel disease or complex narrowing of the coronary arteries and / or a narrowing of the large coronary arteries in the origin, the so-called main stem stenosis, is a clear indication for coronary artery bypass surgery. In 2019, 50,114 isolated and combined bypass operations were performed nationwide (2018: 51,941). In principle, there is no maximum patient age for bypass surgery. Depending on the severity and the location of the stenosis, blood flow to the heart muscle can be improved again in patients of all ages with bypass surgery.
In this group of patients the proportion of people over the age of 70 has increased continuously over the past few years. Last year, approximately 46.7 percent of bypass patients were 70 years and older, with 77 percent of men being significantly higher than women (23 percent), meaning that only every fourth bypass patient was female.
The patient-specific care concept of the bypass operation for coronary artery disease should always be discussed and coordinated in accordance with the currently applicable national and international guidelines in the heart team in order to give the patient a consensus recommendation. The most common cause of CHD is calcification of the arteries, which can lead to severe vasoconstriction and occlusion as the disease progresses, leading to an insufficient oxygen supply to the heart.
Bypass surgery is an extremely complicated surgical operation aimed to restore heart blood flow, bypassing the contraction of vessels. This open-heart bypass surgery is conducted under general anaesthetic. In Russia as well as in Germany during conventional bypass surgery the heart is stopped and an artificial blood circulation apparatus is connected. In recent years minimally invasive techniques have been used in Germany to conduct bypass surgery without stopping the heart and connecting artificial blood circulation apparatus. Advantages of this method are reduction of cell and tissue damage, decrease of blood loss, absence of complications connected with the use of artificial blood circulation apparatus, reduction of surgery duration and considerably quicker rehabilitation process.
Patient’s blood goes to the apparatus which takes up function of lungs and oxygenates blood for some time before it goes back to the vessels. Taking into account the complexity of the surgery, it is crucial not only to find an experienced and knowledgeable surgeon, but also to use advanced medical technologies (e.g., modern blood circulation system minimizing the contact of blood with foreign elements) because breathing with the help of an artificial blood circulation apparatus can have negative influence on patient’s tissues and viscera.
Our homepage offers a brilliant command of information about the best cardiosurgery specialist in Germany, who specialize in bypass operations.
Unfortunately, even in Germany it is not always possible to conduct minimally invasive surgery. In case of serious vessel damage or combined surgical operations (e.g., simultaneous heart valve replacement) it is necessary to stop the heart and to use artificial blood circulation apparatus to conduct the surgery. After the surgery, the patient stays in an in-patient department and is usually discharged in 10-14 days.
Before you consent to this extremely complicated surgery it is important to choose an experienced specialist and a well-equipped clinic. In Germany the bypass surgery is always conducted in accordance with current international standards and is notable for its quality and reliability.
Diagnostics and Preparations
Different kind of diagnostic procedures are used for precise diagnosing and making a final decision on expediency of heart bypass. Coronary catheterization is one of them. During this procedure coronary circulation is examined with introduced catheter using X-rays imaging, which visually represent a whole situation with vascular occlusions, thrombus and plaques, as well as stenosis and aneurysms. Based on the coronary angiograms a cardiologist makes a conclusion to perform CABG or, maybe, balloon angioplasty. Also the common checkup methods are applied as blood tests, electrocardiograms and others.
When it is decided in favor of bypass surgery, it is necessary to prepare the patient for operation. It could take quite a long time. First, the patient should stop using any medications which could cause blood clotting. The smokers should quit smoking. If any unexpected problems occur as flu or inflammation it is strongly recommended to inform a physician because if hidden, those symptoms could affect complications.
When in hospital, the patient stops eating and drinking in a night before the surgery. The doctor also could prescribe some sedative medicaments. Immediately before bypass grafting the patient has given IV anesthesia and, then, goes asleep.
Operational Process
The aim of coronary bypass is to replace diseased arteries with others, which are normally taken from different parts of the patient’s body, as left thoracic artery or the veins removed from the legs and wrists. Depending on how many coronary arteries are bypassed the operation is called single bypass, double bypass etc.
When a patient has received IV and loosen perceptions, a first what a surgeon does is an incision 20-25 cm long in the chest to open the heart for invasion. Then, a heart-lung machine takes oxygen supplying function and, finally, the heart is stopped. After that, a healthy vessel is taken from the body for implantation instead of blocked coronary artery and bypass is made. This action could be repeated a few times. At the end of the procedure, the heart-lung machine is removed and, after checking bypass functioning, the incision is stitched and the patient moves to intensive care unit to be under control of the reanimation team.
Open Heart Bypass Surgery
Open heart bypass surgery or Coronary Artery Bypass Grafting (CABG) is a one of the most demanded cardiac operations intended for those patients who have permanent problems with coronary arteries. Heart bypass normally required when more than one of heart arteries are clotted and it is necessary to create another way for blood flowing to avoid significant discomfort and even mortal risks in patients.
The high-risk group targeted for bypass heart surgery are those who older than 65 years, patients with chronic coronary heart disease, diabetics suffering from heart failure, and those who have multiplied blocked vessels. When coronary lumen has been decreased due to the different reasons including sclerosis or thrombosis, a body – and a brain especially – does not have sufficient blood supply, that can cause serious problems.
Minimally Invasive Bypass Surgery
Generally, aortocoronary bypass always was performed on open heart that is stopped during the operation. But today another option is appeared as alternative to the classical method – minimally invasive surgery. It has advantage that it is less traumatic because, instead of one big breast cut, a few small incisions are carried out and, as a result, recovery period is decreased.
Another advantage is a possibility to operate on beating heart. It is called ‘off pump’ method or coronary revascularization. It always was thought it is better to perform surgical manipulations on motionless heart drained from all the blood, and that still hold true, but there are also some additional risks associated with heart-lung heart machine. Sometimes it is reasonable to use modern technique when veins are harvested through the small cuts by endoscope and, then, they are delivered to the heart also via a few small ports in a patient’s chest by means of special miniature tools.
Though CABG is traditionally associated with open heart surgery, at the moment it is not always so. In any case, a decision, which of the methods to use, normally depends of entire state of the patient’s health, the numbers of diseased arteries and many other related factors as necessity of additional surgery on other parts of the heart, e.g. the valve replacement. It is not possible for patients to determine independently what kind of therapy or surgery they need, so it is better to consult with a qualified specialist. With a choice of clinics in Germany it is easy to find a proper method which is suitable for the patient, taking into account an individual situation and preferences.
Approximate cost of coronary artery bypass surgery in Germany (in EUR)
Coronary artery bypass surgery in Germany is guaranteed to treat patients from stenocardia and short breath. On the following day after the surgery patients already feel better; they can get up from the bed and walk. The cost of the surgery ranges from 18 000 to 30 000 euro. It is often necessary to conduct coronarography before the surgery (from 2000 euro).
Specialized German clinics will provide you with consultations of highly skilled doctors and quality treatment. Individually selected methods of diagnostics, therapy and surgical operations are conducted with the help of ultra-modern medical equipment. Our Friedrichshafen clinic also ensures high standards of hygiene and medical care as well as courteous staff. Health is the most important thing in everyone’s life. Trust us and we will take good care of it!
























 Loading ...
Loading ...


